Could Neuropathy Cause Hammertoes
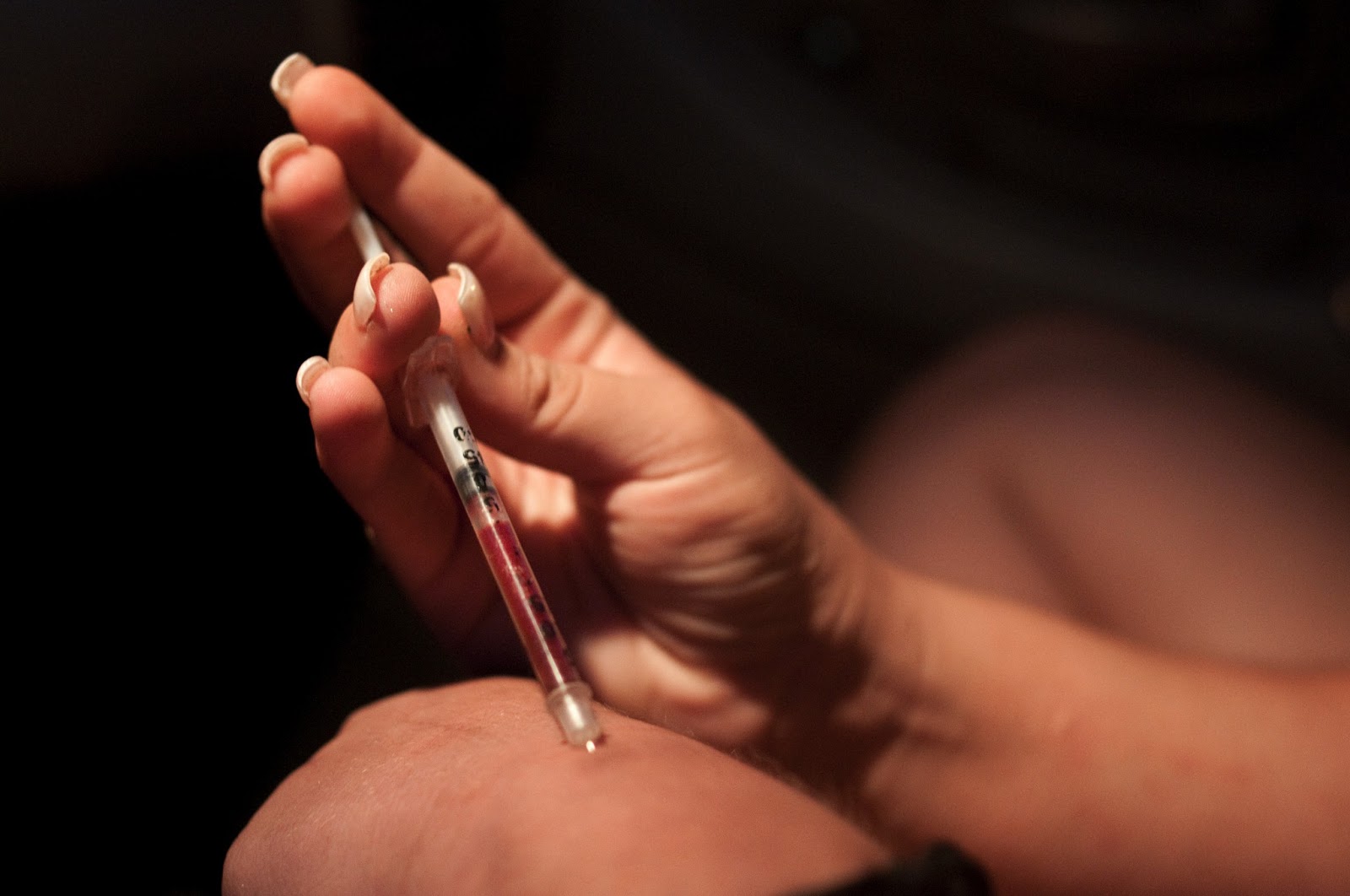 Overview
Overview
A Hammer toe is a deformity of the second, third or fourth toes. In this condition, the toe is bent at the middle joint, so that it resembles a hammer. Initially, hammer toes are flexible and can be corrected with simple measures but, if left untreated, they can become fixed and require surgery. People with hammer toe may have corns or calluses on the top of the middle joint of the toe or on the tip of the toe. They may also feel pain in their toes or feet and have difficulty finding comfortable shoes.
Causes
Shoes that narrow toward the toe force the smaller toes into a bent upward position. This makes the toes rub against the inside of the shoe, and creates corns and calluses, aggravating the toes further. If the shoes have a high heel, the feet are forced forward and down, squeezing the toes against the front of the shoe, which increases the pressure on the toes and makes them bend further. Eventually, the toe muscles become unable to straighten the toe.
 Symptoms
Symptoms
The symptoms of hammertoe include a curling toe, pain or discomfort in the toes and ball of the foot or the front of the leg, especially when toes are stretched downward. Thickening of the skin above or below the affected toe with the formation of corns or calluses. Difficulty finding shoes that fit well. In its early stages, hammertoe is not obvious. Frequently, hammertoe does not cause any symptoms except for the claw-like toe shape.
Diagnosis
The exam may reveal a toe in which the near bone of the toe (proximal phalanx) is angled upward and the middle bone of the toe points in the opposite direction (plantar flexed). Toes may appear crooked or rotated. The involved joint may be painful when moved, or stiff. There may be areas of thickened skin (corns or calluses) on top of or between the toes, a callus may also be observed at the tip of the hammertoe affected toe beneath the toenail. An attempt to passively correct the deformity will help elucidate the best treatment option as the examiner determines whether the toe is still flexible or not. It is advisable to assess palpable pulses, since their presence is associated with a good prognosis for healing after surgery. X-rays will demonstrate the contractures of the involved joints, as well as possible arthritic changes and bone enlargements (exostoses, spurs). X-rays of the involved foot are usually performed in a weight-bearing position.
Non Surgical Treatment
If the toes are still mobile enough that they are able to stretch out and lay flat, the doctor will likely suggest a change of footwear. In addition, she may choose to treat the pain that may result from the condition. The doctor may prescribe pads to ease the pain of any corns and calluses, and medications ranging from ibuprofen to steroid injections for the inflammation and pain. Other options for non-surgical treatments include orthotic devices to help with the tendon and muscle imbalance or splinting to help realign the toe. Splinting devices come in a variety of shapes and sizes but the purpose of each is the same: to stretch the muscles and tendon and flatten the joint to remove the pain and pressure that comes from corns.
Surgical Treatment
Surgery is used when other types of treatment fail to relieve symptoms or for advanced cases of hammertoe. There are several types of surgeries to treat hammertoe. A small piece of bone may be removed from the joint (arthroplasty). The toe joint may be fused to straighten it (arthrodesis). Surgical hardware, such as a pin, may be used to hold the bones in place while they heal. Other types of surgery involve removing skin (wedging) or correcting muscles and tendons to balance the joint.
How Do Bunions Start
Overview
 Bunions are common but they can be misdiagnosed. We sometimes assume that any lump at the bottom of the big toe is a bunion. But as the Latin name (hallux valgus) suggests, the hallmark of a bunion is what happens to the toe itself (the hallux) rather than to the joint at its base. In bunions, the toe veers off in a valgus direction, that is, away from the midline. An outcrop of extra bone, or osteophyte, develops as the body tries to protect the exposed surface of the warped first metatarsophalangeal joint (MTP); a fluid-filled sac, or bursa, may also form, which often becomes inflamed. Foot experts are still not entirely agreed about what causes bunions. Genetics and lax ligaments are both implicated; the role of footwear is less clear. All bunion conversations seem to involve someone stating that barefoot tribes people don?t get bunions. This is not true.
Bunions are common but they can be misdiagnosed. We sometimes assume that any lump at the bottom of the big toe is a bunion. But as the Latin name (hallux valgus) suggests, the hallmark of a bunion is what happens to the toe itself (the hallux) rather than to the joint at its base. In bunions, the toe veers off in a valgus direction, that is, away from the midline. An outcrop of extra bone, or osteophyte, develops as the body tries to protect the exposed surface of the warped first metatarsophalangeal joint (MTP); a fluid-filled sac, or bursa, may also form, which often becomes inflamed. Foot experts are still not entirely agreed about what causes bunions. Genetics and lax ligaments are both implicated; the role of footwear is less clear. All bunion conversations seem to involve someone stating that barefoot tribes people don?t get bunions. This is not true.
Causes
Bunions are more common in women than men. The problem can run in families. People born with abnormal bones in their feet are more likely to form a bunion. Wearing narrow-toed, high-heeled shoes may lead to the development of a bunion. The condition may become painful as the bump gets worse. Extra bone and a fluid-filled sac grow at the base of the big toe.
Symptoms
Bunions may cause no pain at first. But as the big toe begins to turn in towards the other toes, people with bunions usually experience redness, pain, swelling, and tenderness in the area around the joint. Pressure inside the joint or from footwear pressing against the bunion may also cause discomfort. As the affected toe curves closer to the other toes on the foot, these toes can become painful as well. Complications of bunions include corns, calluses, hammer toe, and ingrown toenails. Other complications include irritation of the nerves surrounding the bunion area. Excess rubbing of the bunion against the footwear may lead to changes in the skin, resulting in corns or calluses. Hammer toe is a deformity of the toe immediately next to the big toe. A hammer toe is slightly raised and points upwards from the base and downwards at the end of the toe. Ingrown toenails can result from increased pressure from the big toe on the other toes. There may also be a decrease in the amount a person can move the joint affected by the bunion. Irritation of the nerves will feel like burning or decreased sensation.
Diagnosis
Your doctor will be able to diagnose a bunion by asking about your symptoms and examining your feet. You may also have blood tests to rule out any other medical conditions, such as rheumatoid arthritis or gout, although this is rare. Your doctor may refer you to a podiatrist or chiropodist (healthcare professionals who specialise in conditions that affect the feet).
Non Surgical Treatment
Depending on how many of the causative factors are true, a series of exercises to ensure correct alignment and stability of the lower limb should be implemented. Supportive foot wear with correct width and arch support can provide relief -shoes such as ballet flats, thongs (flip flops) and Ugg boots (or slippers) should be avoided. Mobilization of the mid foot to help re-align the toe correctly, and then taping and padding in the shoe to keep the toe in alignment. Taping to help draw the 1st metatarsal back in towards the second and correct any rotation and drop of the 1st metatarsal. Foam padding shaped like a donut to off load the pressure on the outside of the big toe. 
Surgical Treatment
Bunions are painful deformities that develop when your big toe and first metatarsal slide out of alignment. Most of the time, this condition can be managed and your pain relieved using entirely conservative measures. Since this is a bone deformity, however, the problem can?t be truly corrected without a surgical procedure. Surgery for bunions realigns the displaced bones and restores the foot?s normal function.
Prevention
The best protection against developing bunions is to protect and care for your feet every day. Avoid tight and narrow-fitting shoes. Limit your use of high heels. Wear comfortable shoes with adequate space between your longest toe and the end of the shoe. Getting treatment for very flat or very high-arched feet (if you are experiencing symptoms) will give your feet the proper support and help maintain stability and balance.
Overpronation Of The Foot
Over-pronation is very prominent in people who have flexible, flat feet. The framework of the foot begins to collapse, causing the foot to flatten and adding additional stress to other parts of the foot. Therefore over-pronation can often lead to a case of Plantar Fasciitis, Heel Spurs, Metatarsalgia, Post-tib Tendonitis and/or Bunions. There are many causes of flat feet. Obesity, pregnancy or repetitive pounding on a hard surface can weaken the arch leading to over-pronation. People with flat feet often do not experience discomfort immediately, and some never suffer from any discomfort at all. However, when symptoms develop and become painful, walking becomes awkward and causes increased strain on the feet and calves.
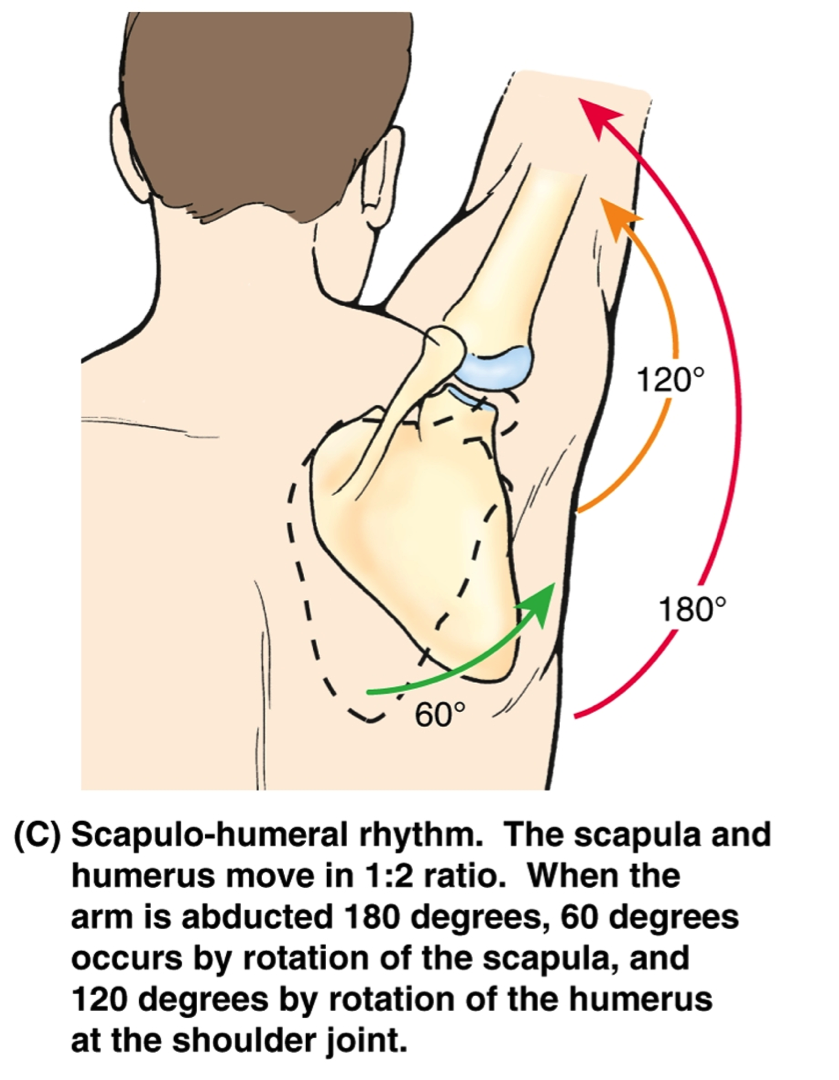
Causes
For those not familiar with the term pronation, you might be familiar with terms related to shoes and pronation such as ?motion control?, ?stability,? and ?neutral cushioned.? The terms motion control and stability are typically associated with the word ?over-pronation? or a foot that is supposedly pronating too much and needs correction. According to the running shoe industry, ?over-pronation? is a biomechanical affliction evident when the foot and or ankle rolls inward past the vertical line created by your leg when standing.
Symptoms
If you overpronate, your symptoms may include discomfort in the arch and sole of foot, your foot may appear to turn outward at the ankle, your shoes wear down faster on the medial (inner) side of your shoes. Pain in ankle, shins, knees, or hips, especially when walking or running are classic symptoms of overpronation. Overpronation can lead to additional problems with your feet, ankles, and knees. Runners in particular find that overpronation can lead to shin splints, tarsal tunnel syndrome, plantar fasciitis, compartment syndrome, achilles tendonitis, bunions or hallux valgus, patello-femoral pain syndrome, heel spurs, metatarsalgia.
Diagnosis
Bunions, calluses and crooked toes may indicate alignment problems. So, it is important to ascertain the condition of a client's toes. Check the big toe to determine if the first joint of the toe is swollen, has a callus or bunion, and/or looks as though it abducts (i.e., hallux valgus) rather than pointing straight ahead. Also, look to see if the lesser toes seem to "curl up" (i.e., the person has hammer or claw toes). This may be indicative of damage to, or inflexibility of the plantar fascia caused by excessive flattening of the foot.
Non Surgical Treatment
Anti-Pronation Insoles provide a unique foot support system that aligns the lower body. The major cause of foot and leg pain is over pronation (rolling over of the feet) which causes excessive pressure on the muscles, ligaments and bones of the lower body. Running insoles treat the underlying cause of over pronation and prevent future occurrences of the associated foot or leg condition. A project conducted at the NIKE Sport Research Laboratory studied the effects of orthotics on rear foot movement in running. Nine well-trained runners who wore orthotics were chosen as subjects. The results of the study indicated that orthotics reduced rear foot movement by roughly one degree or approximately nine percent of the amount found in runners not using orthotics. The average reduction of the maximum velocity of pronation was fifteen percent. Thus this study indicates that orthotics and insoles control over pronation which will treat and prevent many sporting injuries.
Surgical Treatment
HyProCure implant. A stent is placed into a naturally occurring space between the ankle bone and the heel bone/midfoot bone. The stent realigns the surfaces of the bones, allowing normal joint function. Generally tolerated in both pediatric and adult patients, with or without adjunct soft tissue procedures. Reported removal rates, published in scientific journals vary from 1%-6%.
Does Severs Disease Often Necessitate Surgical Procedures?
If you?re a young basketballer/netballer/footballer and have heel pain when playing basketball or sports involving running or jumping, you may have a particular growth pain disorder called Sever?s Disease. It is a condition (not a disease) usually affecting 9-15 year olds that occurs at the back of the heel, where the Achilles tendon attaches to the foot. The Achilles tendon is the tendon connected to the calf muscles. Pulling of the calf muscles results in tension in the Achilles and in adolescents, repeated running/jumping can result in pain and inflammation at the heel, this is called Sever?s Disease.
Causes
There are usually two root causes of Sever?s disease that we?ve found that effect young athletes. Arches are not supported causing a dysfunctional run, jump, and landing. The calves (gastrocnemius and soleus muscles) are overworked, tight, and do not allow proper movement of foot which puts extreme pressure on the Achilles? tendon, in turn irritating the growth plate in the heel.
Symptoms
The typical patient is a child between 10 and 13 years of age, complaining of pain in one or both heels with running and walking. The pain is localized to the point of the heel where the tendo-achilles inserts into the calcaneus (heel bone), and is tender to deep pressure at that site. Walking on his toes relieves the pain.
Diagnosis
Sever's disease is based on the symptoms reported. To confirm the diagnosis, the clinician will examine the heels and ask about the child's activity level and participation in sports. They may also squeeze the back part of the heel from both sides at the same time to see if doing so causes pain and also ask the child to stand on tiptoes to see if that position causes pain. There may be tightness in the calf muscle, which contributes to tension on the heel. Symptoms are usually worse during or after activity and get better with rest. X-rays generally are not that helpful in diagnosing Sever's disease, but they may be ordered to rule out other problems, such as fractures. Sever's disease cannot be seen on an X-ray.
Non Surgical Treatment
Activity Modification: to decrease the pain, limiting sporting activities is essential. Cutting back on the duration, intensity, and frequency can significantly improve symptoms. Heel cord stretching is important if heel cord tightness is present. Heel cushions/cups or soft orthotics decreases the impact on the calcaneus by distributing and cushioning the weight bearing of the heel. Use of NSAIDS. Ibuprofen (Nuprin, Motrin) or naproxen (Aleve) can decrease pain and secondary swelling. Ice. Placing cold or ice packs onto the painful heel can alleviate pain. Short-leg cast. For recalcitrant symptoms a short-leg cast is occasionally used to force rest the heel.
Will Posterior Tibial Tendon Dysfunction Always Call For Surgical Teatments ?
Overview
Have you noticed the arch in your foot collapse over a fairly short period of time as an adult? Or Do you suffer from pain on the inside and sole of your arch? If it does, then you may be suffering from a condition known as adult acquired flat foot. As one of the main support structures of the foot?s arch, the tibilais posterior tendon, along with other muscles, tendons and ligaments, play a very important role in its mechanical function. 
Causes
Posterior tibial tendon dysfunction is the most common cause of acquired adult flatfoot. Sometimes this can be a result of specific trauma, but usually the tendon becomes injured from wear and tear over time. This is more prevalent in individuals with an inherited flat foot but excessive weight, age, and level of activity are also contributing factors.
Symptoms
Pain and swelling behind the inside of your ankle and along your instep. You may be tender behind the inner ankle where the posterior tibial tendon courses and occasionally get burning, shooting, tingling or stabbing pain as a result of inflammation of the nerve inside the tarsal tunnel. Difficulty walking, the inability to walk long distances and a generalised ache while walking even short distances. This may probably become more pronounced at the end of each day. Change in foot shape, sometimes your tendon stretches out, this is due to weakening of the tendon and ligaments. When this occurs, the arch in your foot flattens and a flatfoot deformity occurs, presenting a change in foot shape. Inability to tip-toe, a way of diagnosing Posterior Tibial Tendon Dysfunction is difficulty or inability to ?heel rise? (stand on your toes on one foot). Your tibialis posterior tendon enables you to perform this manoeuvre effectively. You may also experience pain upon attempting to perform a heel rise.
Diagnosis
Examination by your foot and ankle specialist can confirm the diagnosis for most patients. An ultrasound exam performed in the office setting can evaluate the status of the posterior tibial tendon, the tendon which is primarily responsible for supporting the arch structure of the foot.
Non surgical Treatment
A painless flatfoot that does not hinder your ability to walk or wear shoes requires no special treatment or orthotic device. Other treatment options depend on the cause and progression of the flatfoot. Conservative treatment options include making shoe modifications. Using orthotic devices such as arch supports and custom-made orthoses. Taking nonsteroidal anti-inflammatory drugs such as ibuprofen to relieve pain. Using a short-leg walking cast or wearing a brace. Injecting a corticosteroid into the joint to relieve pain. Rest and ice. Physical therapy. In some cases, surgery may be needed to correct the problem. Surgical procedures can help reduce pain and improve bone alignment. 
Surgical Treatment
If cast immobilization fails, surgery is the next alternative. Treatment goals include eliminating pain, halting deformity progression and improving mobility. Subtalar Arthroereisis, 15 minute outpatient procedure, may correct flexible flatfoot deformity (hyperpronation). The procedure involves placing an implant under the ankle joint (sinus tarsi) to prevent abnormal motion. Very little recovery time is required and it is completely reversible if necessary. Ask your Dallas foot doctor for more information about this exciting treatment possibility.
Can You Fix Flat Feet In Adults?
Overview
Painful progressive flatfoot, otherwise known as tibialis posterior tendonitis or adult-acquired flatfoot, refers to inflammation of the tendon of the tibialis posterior. This condition arises when the tendon becomes inflamed, stretched, or torn. Left untreated, it may lead to severe disability and chronic pain. People are predisposed to tibialis posterior tendonitis if they have flat feet or an abnormal attachment of the tendon to the bones in the midfoot. 
Causes
Women are affected by Adult Acquired Flatfoot four times more frequently than men. Adult Flatfoot generally occurs in middle to older age people. Most people who acquire the condition already have flat feet. One arch begins to flatten more, then pain and swelling develop on the inside of the ankle. This condition generally affects only one foot. It is unclear why women are affected more often than men. But factors that may increase your risk of Adult Flatfoot include diabetes, hypertension, and obesity.
Symptoms
PTTD begins with a gradual stretching and loss of strength of the posterior tibial tendon which is the most important tendon supporting the arch of the human foot. Left untreated, this tendon will continue to lengthen and eventually rupture, leading to a progressive visible collapse of the arch of the foot. In the early stages, patients with PTTD will notice a pain and swelling along the inner ankle and arch. Many times, they are diagnosed with ?tendonitis? of the inner ankle. If the foot and ankle are not properly supported during this early phase, the posterior tibial tendon can rupture and devastating consequences will occur to the foot and ankle structure. The progressive adult acquired flatfoot deformity will cause the heel to roll inward in a ?valgus? or pronated direction while the forefoot will rotate outward causing a ?duckfooted? walking pattern. Eventually, significant arthritis can occur in the joints of the foot, the ankle and even the knee. Early diagnosis and treatment is critical so if you have noticed that one, or both, of your feet has become flatter in recent times come in and have it checked out.
Diagnosis
In diagnosing flatfoot, the foot & Ankle surgeon examines the foot and observes how it looks when you stand and sit. Weight bearing x-rays are used to determine the severity of the disorder. Advanced imaging, such as magnetic resonance imaging (MRI) and computed tomography (CAT or CT) scans may be used to assess different ligaments, tendons and joint/cartilage damage. The foot & Ankle Institute has three extremity MRI?s on site at our Des Plaines, Highland Park, and Lincoln Park locations. These extremity MRI?s only take about 30 minutes for the study and only requires the patient put their foot into a painless machine avoiding the uncomfortable Claustrophobia that some MRI devices create.
Non surgical Treatment
Orthoses (insoles, functional orthoses, ankle supports, braces, ankle foot orthoses (AFOs)) - are usually custom-made to increase the functional stability of the foot and improve the mechanical properties of the tendon as well as reducing the actual degree of strain on the tendon. This reduces pain and inflammation. Physiotherapy - exercises and physiotherapy are often used to increase mobility, strengthen the tendon itself, stretch your Achilles tendon as well as reduce pain. Once the tendon has been stretched (stage one), the heel starts rolling outwards. Total immobilisation in a cast may help the symptoms to subside and prevent progression of the deformity in a smaller percentage of patients. Long-term use of orthoses may help stop progression of the deformity and reduce pain without surgery. Non-surgical treatment is unlikely to prevent progression to stage three and four but may be chosen by some patients who either are unsuitable for surgery or prefer not to have surgery. 
Surgical Treatment
Flatfoot reconstruction (osteotomy). This is often recommended for flexible flatfoot condition. Flatfoot reconstruction involves cutting and shifting the heel bone into a more neutral position, transferring the tendon used to flex the lesser toes (all but the big toe) to strengthen the posterior tibial tendon, and lengthening the calf muscle. Fusion (also known as triple arthrodesis). Fusion involves fusing, or making stiff, three joints in the back of the foot the subtalar, talonavicular, and calcaneocuboid joints, to realign the foot and give it a more natural shape. Pins or screws hold the area in place until it heals. Fusion is often recommended for a rigid flatfoot deformity or evidence of arthritis. Both of these surgeries can provide excellent pain relief and correction.
Heel And Arch Pain
Pain in arch of foot, a very common problem for millions of people worldwide who are suffering from this ailment every single day. Whether it's arch pain, heel pain, bunion pain, big toe pain, little toe pain or anything else in between, sore feet are no fun! It's no denying that if your feet aren't right, you feel out of sorts. In this article you will discover the possible causes of the pain in the arches of your feet and common treatments and solutions. Often linked with heel pain, pain in the arch of the foot is very common, particularly in those that spend a lot of time on their feet and those that play sports regularly.

Causes
Flatfoot can have many different causes. It could be a weakness or a structural abnormality you?ve had since birth. It could also mean that tendonitis, damage to the connective tissues, arthritis, or nerve problems have affected the structures in your feet. Even wearing unsupportive footwear can lead to weakness and arch pain. Whatever the cause, many conservative, noninvasive treatments exist to help relieve and eliminate your discomfort.
Symptoms
The foot of a newborn with congenital vertical talus typically has a convex rocker-bottom shape. This is sometimes combined with an actual fold in the middle of the foot. The rare person who is diagnosed at an older age often has a "peg-leg" gait, poor balance and heavy calluses on the soles where the arch would normally be. If a child with congenital vertical talus has a genetic disorder, additional symptoms often are seen in other parts of the body.
Diagnosis
Your doctor may order imaging tests to help make sure your heel pain is caused by plantar fasciitis and not another problem. X-rays provide clear images of bones. They are useful in ruling out other causes of heel pain, such as fractures or arthritis. Heel spurs can be seen on an x-ray. Other imaging tests, such as magnetic resonance imaging (MRI) and ultrasound, are not routinely used to diagnose plantar fasciitis. They are rarely ordered. An MRI scan may be used if the heel pain is not relieved by initial treatment methods.
Non Surgical Treatment
In addition to relieving the pain by providing better metatarsal support for your feet, many doctors advise stretching and strengthening the muscles that surround the damaged or weakened tendons. This advice can prove especially effective in preventing the possible side effects of fallen arches, including: inflammation and discomfort in the ligaments of the sole, Achilles tendonitis, shin splints, calluses, and bunions. Like plantar fasciitis, left untreated, fallen arches can cause a domino effect that impacts your legs, hips, and back.

Surgical Treatment
The main goal of surgery is to reduce pain and improve function. It may also reduce other injuries such as repeated ankle sprains and broken bones. Surgery may be considered if there is no relief with physical therapy, changes in shoewear and/or changes in activity. Some patients will also have tendon problems, ankle weakness and foot fractures. These patients may require other procedures to address related problems. If you have medical problems that make surgery unsafe, any infections or blood vessel disease, cavus foot surgery may not be appropriate. The surgical procedures involved with the correction of the cavus foot are varied. Theses may include correction of the bony deformity, ankle looseness and the muscle imbalances that cause the deformity. The goal is to provide a foot that evenly distributes weight along both inside and outside edges. A variety of incisions may be needed to perform the procedures related to the correction of the cavus foot.
Prevention
It is possible to prevent arch pain by wearing well-fitting shoes while performing any physical activity. Many times doctors will suggest a therapeutic shoe with a higher heel to relieve the pressure on the achilles tendon and also the arch muscle (plantar fasciitis). People with arch pain suffer from regular flare-ups of pain. However there is no risk to others as this is not a contagious condition.